This story first appeared at ProPublica. ProPublica is a Pulitzer Prize-winning investigative newsroom. Sign up for The Big Story newsletter to receive stories like this one in your inbox.
Vicky Rae Byrd had a sinking feeling.
As she scrolled through her phone on election night, her pick for president — Joe Biden — seemed to have a slight edge. Byrd was too stressed to turn on the local news. Her husband sat down with her in their living room, and the couple settled on some sitcom.
Montana had long voted Republican in presidential elections. But it had a Democratic governor for the past 16 years, and that was almost certain to end. Ending with it, Byrd feared, would be the state’s aggressive response to COVID-19.
Byrd, 58, with long silver hair, had been sounding early warnings as director of the Montana Nurses Association, which lobbies for the state’s 18,000 nurses, many of them unionized. She’d been a nurse herself for 33 years, most of them at St. Peter’s Health in Helena, working in pediatric cancer.
“Nurses are really good at foreseeing,” she recalled. “I’m like, shut down before it gets here! Then, one case gets here, and I’m like: ‘Shut down, hold down the state. Keep me safe.’”
By that fall, many voters were fed up with departing Gov. Steve Bullock’s mask mandate and stay-at-home order. Small businesses complained they were suffocating, Montana’s economy was struggling and efforts to control the virus were colliding head-on with the state’s deeply ingrained belief in personal freedom.
As election night wore on, Byrd kept sneaking glances at her phone. She saw votes piling up for the Republican candidate, multimillionaire businessman Greg Gianforte, who was running against Bullock’s lieutenant governor, Mike Cooney. A Donald Trump acolyte who’d gained national attention for pleading guilty to assaulting a reporter on the eve of his 2017 election to Congress, Gianforte had called for the speedy development of COVID-19 vaccines but answered few questions about how he’d fight what he called “this invisible enemy.” He had, however, made it clear he supported personal responsibility over mandates.
Days after a decisive victory, Gianforte appointed a 21-member panel to guide him on COVID-19. Determined to recharge the economy, his wide-ranging picks included a refinery executive, a local Best Western operator and the owner of a pizza restaurant and casino. Dr. Scott Gottlieb, the former commissioner of the federal Food and Drug Administration, added national gravitas.
Missing from the long list of names were any officials from the state public health agency who had been running the COVID-19 response. Among them was Jim Murphy, a veteran of almost 33 years at the state’s Department of Health and head of its communicable diseases division.
Under Bullock, Murphy had helped deliver daily COVID-19 updates. But in conference calls with the governor-elect’s office and the new coronavirus panel, he sensed “pretty much instantly” that public health was not the priority. The calls, Murphy remembered, “focused more on the perceived overresponse” to COVID-19.
(Gianforte declined requests for an interview, and his press secretary, Brooke Stroyke, said she wouldn’t respond to “biased, gotcha” questions about the governor’s actions, which she said have been “widely covered.”)
One conference call turned tense when the head of the task force, a conservative former state senator named Kristin Hansen, questioned Murphy about the validity of state data on COVID-19 infections and deaths.
“Some of us spoke up to offer the public health side of the story,” Murphy recalled. “That wasn’t always well received.”
When Gianforte took office on Jan. 4, 2021, Montana had avoided the worst of the pandemic. About a thousand residents had died, slightly less per capita than the national average. And the state had just started rolling out vaccines under a plan worked out by Murphy and his team.
Almost immediately, Gianforte began rolling back COVID-19 restrictions. He won applause from businesses by lifting Bullock’s order restricting their hours. A month later, amid a lull in the state’s COVID-19 cases, he allowed an indoor mask mandate to expire; state medical officer Dr. Greg Holzman resigned the next day.
Gianforte got his first Pfizer shot the day he opened vaccines to all adults, weathering criticism from some far-right conservatives for calling the shots “safe and effective.” But even as Montana’s vaccination rate began to sputter, Gianforte again emphasized that getting vaccinated was a personal choice.
As Byrd watched Gianforte with concern, she and her small staff were also trying to track Montana’s GOP-controlled Legislature as it considered a flurry of public health measures. One that initially escaped her attention was introduced by a new legislator, Rep. Jennifer Carlson.
Carlson had pressed the Legislature even before COVID-19 to do away with vaccine mandates. The mother of five, who has a biomedical science degree, had given all of her kids the typical childhood vaccinations. But one child, she recalled, had suffered a severe reaction. Soon after she took office, Carlson introduced legislation that she said she got help drafting from the leader of a popular Facebook group, Montanans for Vaccine Choice.
Her legislation gave the unvaccinated standing as a “protected class,” making it illegal to discriminate against them. No employers could require vaccinations of any kind. The language covered all vaccines, including measles, mumps and other standard childhood vaccinations.
There were no exemptions for people working at hospitals.
The legislation worried Murphy. But he said that the governor’s office told him and other state health officials to stay out of the debate.
“We were told we had to be neutral,” Murphy recalled.
The bill caught fire, particularly after a hospital in Great Falls announced its plan to terminate unvaccinated employees. Gianforte, responding to complaints from alarmed hospitals and other health care providers, sent amendments back to the Legislature that he said “strengthened” the bill. It would at least allow hospitals to ask employees if they were vaccinated so they could make adjustments. But if unvaccinated staffers felt they were being discriminated against, they could sue.
The amended bill sailed through the GOP-heavy House and Senate in the session’s final days. Gianforte signed HB 702 into law on May 7, the same day he signed another bill restricting the authority of local public health agencies to impose COVID-19 restrictions.
Carlson told ProPublica she was quickly deluged with calls. Legislators in other states asked how she had pulled off a “miracle.” Other callers left messages saying she would be responsible for more deaths.
“Nobody wants to be called anti-vax. Nobody wants to be accused of killing grandma,” she said. “I honestly don’t think the government should be in charge of your lives.”
The Montana Medical Association and others sued in federal court, arguing that health care providers receiving federal funding are required to vaccinate their workers. Byrd’s group joined the suit. She noted in an affidavit that when St. Peter’s hired her, it required proof of vaccination “as a condition of employment.”
Byrd remembers thinking: “I don’t go to the governor’s office for my colonoscopy. Certainly you shouldn’t go to the governor’s office to have him lecture you on what immunizations you should or shouldn’t get.”
The Surge
By July, less than three months after Carson’s bill became law, the delta variant began to spread across Montana.
Vaccine hesitancy remained high. Early in the pandemic, residents of the state capital, Helena, stopped at 8 p.m. to howl at the moon in a salute to health care workers. Now staffers faced verbal, even physical abuse, often over intake questions about vaccination status and wearing masks.
St. Peter’s posted a warning in the entryway “Aggressive Behavior Will Not be Tolerated.” Almost overnight, nurses “went from heroes to zeros,” Byrd said.
Gianforte warned that delta was highly contagious and urged citizens to protect themselves, but he again emphasized there would be no mandates.
St. Peter’s doctors and nurses signed a letter on Sept. 1 pleading with Montanans to get vaccinated. One of them was Charlotte Skinner, a nurse and a mother of two who works in the St. Peter’s emergency room and is an officer in the hospital’s nurses union. Earlier in the pandemic, Skinner had volunteered to appear at a press conference with Bullock, where she delivered an impassioned speech calling for an end to “partisan bickering” and urging the state to “embrace science.”
Afterward, a friend warned Skinner not to look at her Facebook messages. She peeked in to find “shocking stuff,” she recalled, including one commenter who “said he wanted to scalp me and my family.”
Vaccines remained a flashpoint even among staffers, about a quarter of whom declined to get one. Skinner said word spread quickly nationwide that Montana was a state where unvaccinated medical workers could work with legal protections. Perhaps unintentionally, she said, it became a “recruiting tool.”
By early September, COVID-19 hospitalizations were climbing quickly. Hospitals in Billings and Missoula warned they were overloaded. Non-COVID-19 patients were competing with COVID-19 patients for resources. The critical care units at St. Peter’s were at 100% capacity.
At St. Peter’s request, Gianforte sent National Guard troops to help, detailing 10 guard members to the 99-bed hospital. Among their tasks was helping exhausted nurses flip struggling COVID-19 patients onto their stomachs so they could breathe more easily. Staff scrambled to deliver ICU-level care in other units as beds dwindled.
By then, despite his state’s unfolding calamity, Gianforte had said on Twitter that Montana would take the vaccine fight national by challenging what he called Biden’s “unlawful and un-American” vaccine mandate.
St. Peter’s was so crowded that nurses had little time to spend with patients, even in the ICU. “Turn. Make sure the vents are on. Go on to the next person,” as Byrd described it.
To handle surges, Montana’s state health agency had revised its guidance on when a hospital should declare “crisis standards of care,” a designation that protects overwhelmed facilities from liability when they can no longer offer normal services and must consider rationing care.
A state official announced the directives on Sept. 15, saying he hoped hospitals would never have to use them.
One day later, St. Peter’s president and chief medical officer, Shelly Harkins, called a video press conference. The hospital was already meeting all of the criteria — long emergency room wait times, scarce equipment and medications, and no vacant beds, including in its eight-bed ICU.
A former Air Force physician, Harkins joined the hospital in 2017 after running a health system in Indiana. Harkins had a light-hearted side. She had played keyboard in a band called Leather Moose. But now, Harkins delivered the blunt reality.
COVID-19 patients filled every available bed, and St. Peter’s was running out of medication to treat them. The hospital was splitting up doses of some medications between patients and using seven times its normal amount of propofol, a sedative that can help ease the agony of the terminally ill.
Harkins was invoking “crisis standards of care,” she said. She was clear about what patients and their families could expect to see. “We are giving our staff permission to not do it all. The hardest thing they will do in their careers is not giving the care they are used to giving, but they simply can’t.”
“JEEZ!” someone in the background exclaimed.
Crisis standards would impact not just COVID-19 patients but anyone needing care. Some decisions would require a kind of battlefield triage, applying standards that had been crafted by a national advisory board in 2009 after the H1N1, or swine flu, epidemic. The guiding principle would be to try to save the greatest number of lives. That could mean giving a scarce resource, like an ICU bed or a ventilator, to a person thought to be most likely to survive.
The prospect of rationing health care has long terrified Americans. Republicans used it as a pillar of an early fear-mongering campaign against President Barack Obama’s Affordable Care Act, when Sarah Palin and then others falsely claimed the legislation would create “death panels.”
Harkins’ work in family medicine and palliative care had prepared her to be direct but reassuring. “We are still very much here to provide care to our community, and we are doing absolutely all we can to keep all services open,” she added during the announcement. “True emergencies will always receive priority.”
But the strain on St. Peter’s staff of 1,700 was escalating. Instead of monitoring one or two desperately ill COVID-19 patients, nurses were caring for five or six.
Byrd’s association set up an email inbox for nurses to anonymously vent. “I no longer look forward to what impact I might make every shift. Instead, I steel myself to simply survive another day at the bedside without breaking down in front of the patients,” wrote one.
Harkins said that the hospital had more than 200 staff vacancies at the time. She told ProPublica the hospital was short of staff throughout.
When COVID-19 first began its march across America, the hospital had set up a 13-member Scarce Resources Committee to help doctors wrestle with tough decisions if things ever got bad. It included doctors, administrators and the hospital chaplain.
It was only called twice in nearly a year and a half. After delta hit, the committee convened six times in just over a month.
The Call
Around lunchtime one day in the middle of October, Harkins got an urgent text from an emergency room doctor.
“I need help,” the doctor pleaded.
A COVID-19 patient with dangerously low oxygen levels had just arrived by ambulance. The woman was severely obese, which put her at high risk. “As soon as she hit the room, we knew if we don’t act rapidly she will be dead soon,” recalled the ER doctor, who later spoke with ProPublica on the condition of anonymity.
The doctor wanted to transfer the patient to the ICU. But the unit was full.
Harkins quickly convened a video meeting of the Scarce Resources Committee. As doctors began to weigh in, the committee realized the crisis ran deeper. There were an additional four critically ill patients in other parts of the hospital who also should be transferred to the ICU.
The math was brutal: Five patients and zero beds.
The committee began the process spelled out by an allocation algorithm in Montana’s crisis standards of care guidelines. Factors like age and preexisting conditions were fair to consider, but vaccination status was not.
Harkins quarterbacked as the committee deliberated: How old? Other serious health conditions? How long in the hospital?What is the latest status?
One critically ill non-COVID-19 patient had a serious heart condition. “I feel the heart patient will not survive. How do you feel?” one doctor asked. Everyone agreed that the heart patient would not get an ICU bed and could be treated in another unit.
After about 20 minutes, the committee decided the woman in the emergency room had the most urgent need and should go to the ICU. They could make a bed available by moving a dying patient too ill to survive to another unit. But they had promised the patient’s family they would wait until everyone arrived to say their goodbyes before removing life support. One family member was not there yet. The hospital was running out of time.
Suddenly, a piercing code blue alarm sounded in the emergency room. “Wait a minute, guys,” an attending physician told the committee. “The patient is coding.”
Then, “the patient has died.”
The committee took a moment to absorb the news. Then it began deliberating again. The call lasted an hour. In the end, the terminal ICU patient’s family members were able to gather to say their goodbyes. When that bed was free, another patient discussed during the call was moved into the ICU but died a few days later.
Of the five patients who had been vying for a bed, four ultimately died.
“Under normal circumstances we would have moved all five into the ICU,” Harkins later told ProPublica. “But we just couldn’t.”
Being forced to make such profound decisions changed Harkins and others on the call.
Kimberly Pepper, the hospital chaplain who served on the committee, described seeking solace in the “thin places,” a Celtic belief that there are spots where the distance between heaven and Earth is at its slimmest. Hers was in the Montana mountains. She noticed her hikes had become longer and longer.
Harkins said hospital staff had found their “cry spots” to deal with the anguish. Hers was in an empty office.
“The human psyche,” she said, ”was not built for this.”
The Patients
The virus was forcing cracks in the hospital’s usual care.
Nurses at St. Peter’s had to bathe patients and clean rooms to make up for the large number of nursing assistants who had quit. Kari Koehler, who was serving as the acting chief of nursing during the surge, told ProPublica that the exodus had left the hospital with two assistants per shift instead of the desired 10.
Donna Burrell, a 66-year-old grandmother and former Little League president who worked as a clerk for the Helena school district, arrived at St. Peter’s emergency room in early September with COVID-19-related respiratory failure. A doctor called her daughter, Kima Rosling, to explain that ICU space was unavailable and “may be limited elsewhere throughout the state,” according to medical records.
For Rosling, the next days were chaotic. Burrell was transferred to the ICU when her oxygen levels dropped, then transferred back to a step-down unit.
A doctor prescribed a medicine to control Burrell’s high blood sugar, which can lead to stroke, heart attacks or kidney failure. But a doctor’s note in her file said the order “did not go through” at first and the condition escalated.
Burrell was also having trouble keeping on her oxygen mask. A doctor noted in her records that he told her family “we are in no position to ensure that she keeps it on 24 hours a day.” The medical team told the family it would have to step in to help.
Burrell kept asking doctors when she could go home, and the family discussed transferring her to a rehab facility. But her condition took a sudden turn. Burrell told her daughter and husband that she fell and hit her head during the night while trying to walk to the bathroom.
There was no notation of a fall in Burrell’s record, and Rosling said she complained to a head nurse. Nursing notes show that Burrell was placed on a bedpan.
Burrell’s oxygen levels declined and soon she was back in the ICU, her organs failing. Rosling knew her mother wanted to fight to stay alive and gave doctors permission to intubate her.
But Burrell died at 6:24 a.m. on Oct. 7, after a month of treatment.
Rosling said she realizes that her mother came into St. Peter’s at a terrible time, but she believes her care was lacking and that the medical team should have treated the fall more seriously. Rosling said tracking her mother’s care was a “day-to-day war.”
St. Peter’s administration declined to comment on treatment of individual patients, citing privacy laws. But the hospital said that even amid the chaos, it offered quality care to all patients.
Family members of other patients told ProPublica that it was clear the hospital was under stress. Alarms seemed to be beeping endlessly and medical staff were visibly fatigued. Doctors sometimes told them that drugs and beds were in short supply. The chaos, the family members said, only heightened the anxiety of having a loved one in the hospital and, in some cases, their grief.
Jodi Raue said her concern over her 84-year-old mother’s swift decline after a serious fall was made worse by a lack of communication with doctors about their decision to move her mother out of the ICU. While her mother had a do not resuscitate order signed several years earlier, Raue remains upset that her mom’s last days were not more orderly and peaceful.
“I don’t know why they didn’t tell me,” Raue said. “It wouldn’t have changed anything for my mom, but it would have been transparent.”
Harkins said in a statement earlier this year that the hospital tried to keep families in the loop about treatment decisions, but it depended on individual circumstance and situation, especially during the crisis.
“We are confident,” Harkins wrote, “that our actions helped us focus on the most important task at hand: saving lives.”
The Politics
As overwhelmed doctors and nurses struggled to keep their patients alive, Montana’s red state politics pushed their way into the hospital.
On Oct. 10, St. Peter’s admitted 81-year-old Shirley Herrin, an iconic figure in state GOP politics who had supervised secretaries for Republicans in the Montana Senate. St. Peter’s was treating her for COVID-19, but Herrin’s daughter, Susan Williams, objected to the treatment.
Williams wanted her mother sent home where she could take ivermectin and hydroxychloroquine, drugs then widely promoted as possible treatments by right-wing media and President Donald Trump. She accused St. Peter’s of declining to discharge her mother and of blocking the paperwork needed to give her medical power of attorney. (The hospital later denied this.)
St. Peter’s refused to prescribe the unproven drugs. But Herrin’s daughter wouldn’t back down.
Williams said she and an aunt got ivermectin tablets, typically used to treat parasites, from an outside physician and dissolved them into a frozen drink — a “Frostie.” A nurse delivered the concoction, not knowing it was spiked, to Herrin’s bedside for five days before discovering it.
Later, after Williams confronted staff about moving her mother to another room without explanation, a doctor called hospital security. Williams was asked to leave the building and retreated to the parking lot, where she called a top official in the Montana attorney general’s office, Kristin Hansen.
Hansen was the same politician who had been head of Gianforte’s COVID-19 task force and questioned the state’s statistics. She jumped into action.
Hansen dispatched a Montana Highway Patrol trooper to the hospital, according to a later state report, and the trooper interviewed Williams. Hansen also called a friend near Herrin’s bedside. The friend put the call on speaker and hospital staff heard Hansen warning that St. Peter’s could face “legal ramifications.” More pressure came from a former Republican state senator, who called the hospital to complain about Herrin’s treatment.
The attorney general himself, Austin Knudsen, contacted a hospital lobbyist to set up a phone call with St. Peter’s CEO and other top administrators. He texted a hospital board member that he was ready “to send law enforcement in and file an unlawful restraint charge.”
From her hospital bed, Herrin wrote to her doctor asking that Williams be allowed to give emotional comfort. In Herrin’s final hours, her daughter said she rubbed her feet with an ivermectin salve. Herrin died Oct. 26.
After the attorney general’s actions were reported by the Montana State News Bureau, Knudsen’s press secretary issued a statement defending his office. Knudsen told a local reporter the notion that his office had abused its authority was “absolute, utter nonsense.”
A spokesperson from the attorney general’s office told ProPublica a state report “made it clear” that neither Knudsen nor Hansen threatened anyone.
The hospital said in a statement to ProPublica: “These officials have no medical training or experience, yet they were insisting our providers give treatment for COVID-19 that are not authorized, clinically approved, or within the guidelines established by the FDA and the CDC. In addition, they threatened to use their position of power to force our doctors and nurses to provide this care.” (Read the full statement).
It’s not clear what became of the attorney general’s inquiry into St. Peter’s, but the spokesperson said Williams’ complaint about St. Peter’s “is still under review.” Hansen asked an investigator from the fraud division to look into the matter. Williams also said she met with Knudsen in his office in late April. The county sheriff authorized an autopsy of Herrin.
Williams, who gained local attention with a talk radio interview on her mother’s case, insists that St. Peter’s withheld lifesaving treatment — and tried to push her to expensive therapies. She told ProPublica she still blames the hospital for her mother’s death.
The Lessons
What happened at St. Peter’s fits a broader national pattern that researchers are only beginning to understand as the virus continues to mutate and spread. Americans have died not simply from COVID-19 but also potentially from gaps in care that the pandemic caused.
One study last year found as many as 1 in 4 COVID-19 deaths early in the pandemic may have been due to strained hospital resources rather than the infection itself. One of the study’s authors, National Institutes of Health clinician and researcher Dr. Sameer S. Kadri, noted at the time it was a “truly humbling statistic.”
Kadri told ProPublica recently that, on reflection, the study’s shocking finding is “probably an underestimate.” Avoidable deaths also may have included people hospitalized for other problems, like heart attacks and trauma.
A study from this year found particularly higher mortality rates among those treated in rural hospitals, smaller hospitals and hospitals not affiliated with medical schools.
Experts say part of that can be attributed to overstretched staff and not enough medical resources to go around. “We’ve had increased mortality because of microdecisions,” said Dr. David Scales, a sociologist and practicing physician at Weill Cornell in New York.
A hospital can often guard against risks because it has many layers of defense, arranged “like Swiss cheese,” said Scales, who studies patient safety. But “sometimes the holes line up” and accidents occur. “If you are admitted to the hospital while it’s overwhelmed, you’re at higher risk.”
Hospitals can lower that risk. The Cambridge Health Alliance, which runs two hospitals north of Boston, has won attention for its proactive approach to handling its own COVID-19 surge in the spring of 2020. It moved rapidly to set up a coordinating COVID-19 Incident Command System, expanded its ICU beds into other hospital wards and redeployed large numbers of staffers.
Dr. Maren Batalden, the hospitals’ chief quality officer, said Republican Gov. Charlie Baker backed them up by issuing an order suspending nonessential services. Later, when vaccines became available, Baker issued an order mandating them — with religious and health exemptions — for all state executive department employees and nursing home staff.
“We had the opposite of anti-vaccination. We had vaccine mandates,” Batalden said.
COVID-19 is a common enemy, but it has struck a divided nation. “Ideally, we would have bound ourselves together to protect ourselves and one another,” Batalden said. “Instead, in many places, the virus illuminated and heightened our divisions, exposing the fact that our lack of social cohesion makes us collectively vulnerable.”
A growing body of research shows that death rates were significantly higher in red states like Montana because of lower vaccination rates.
William Hanage, an epidemiologist and researcher at the Harvard T. H. Chan School of Public Health, said that “political lean” has emerged as one of the best indicators for COVID-19 death rates — as much as obesity or advanced age.
“Viruses don’t care how you vote,” he said. “If you allow lots of people to become infected at once, it will crash health care.”
One recent study by the Brown University School of Public Health and others estimated that 1,464 Montana COVID-19 deaths — about 1 in 3 — could have been prevented if every eligible adult had been vaccinated.
“Montana is a very good example of a state that has seen consistent undervaccination, and as a result every third life could have been saved,” said the study’s co-author Stefanie Friedhoff, associate professor of health services, policy and practice at the Brown University School of Public Health.
Harkins, the St. Peter’s chief medical officer, is a lifelong Republican. She calls herself “MAGAfan” on Instagram. But she has seen divisions in her own family over the need for vaccines. It’s exhausting and heartbreaking. “It didn’t have to be like this,” she said. “Conservatives are on the wrong side of this.”
The Aftermath
The surge at St. Peter’s hospital has long since receded. But a residue of distrust remains. Some families say they have not fully recovered and blame the hospital for substandard care. There is no evidence that medical care at St. Peter’s was any worse than at any other hospital hit by the delta surge, and data about patient care is still unavailable.
“In retrospect, there is no denying that it was an unprecedented time, the hardest most of us have seen in our careers,” said Harkins in a recent emailed statement in response to questions from ProPublica. “But we cannot understate how our caregivers’ response, sacrifice, and willingness to share their time and talents saved many local lives.”
Meanwhile, Gianforte and his attorney general, Knudsen, have continued fighting the Biden administration’s vaccine policies. Gianforte sent a letter to unvaccinated health care workers in February encouraging them to consider using religious exemptions from vaccine requirements.
Murphy left his state health department job in June 2021 and charged later that Gianforte’s office had nixed an outreach campaign to get teenagers vaccinated. Murphy and other health officials and experts launched a private effort to promote student vaccinations.
“I’m a little frustrated and a little discouraged by what I see in some of our political leadership,” Murphy said. “They’re patronizing people because it’s necessary to get their votes, instead of taking the time and educating the population about why we need to do some of the things we need to do.”
Bullock, who lost his 2020 bid for a U.S. Senate seat and now serves as court-appointed monitor over Purdue Pharma, still remembers the days when as governor, he knew the location of every available ventilator in the state, the daily death toll and the number of infections. He talked weekly to anxious governors from both political parties who, despite different leadership styles, were equally desperate for solutions.
He recently watched his parents recover from COVID-19 and knows that the virus is not over. The challenge, he said, is to minimize politics. “Do the best you can, informed by science advisers, and whether you like it or not, that’s what you signed up for,” he said of a governor’s role.
An ongoing federal court case will decide whether unvaccinated Montana health care workers are protected from federal mandates if they work at facilities funded by the federal Centers for Medicare and Medicaid Services.
Byrd, who just recovered from a mild second bout with COVID-19, and other plaintiffs won a small victory in March when a federal judge enjoined a key provision of Montana’s anti-vaccination law, saying it could do “irreparable harm” to physician’s and provider’s offices.
In a pointed Facebook message, one state lawmaker warned Byrd’s association to drop the lawsuit and “don’t mess with the will of the legislature.”
In June, the head of Montana’s state health agency stepped down, and Gianforte replaced him with a former lobbyist and Republican congressional staffer.
Montana’s vaccination rate remains well below the national average. In the latest CDC data, just under 58% of residents are fully vaccinated, ranking 39th in the nation.


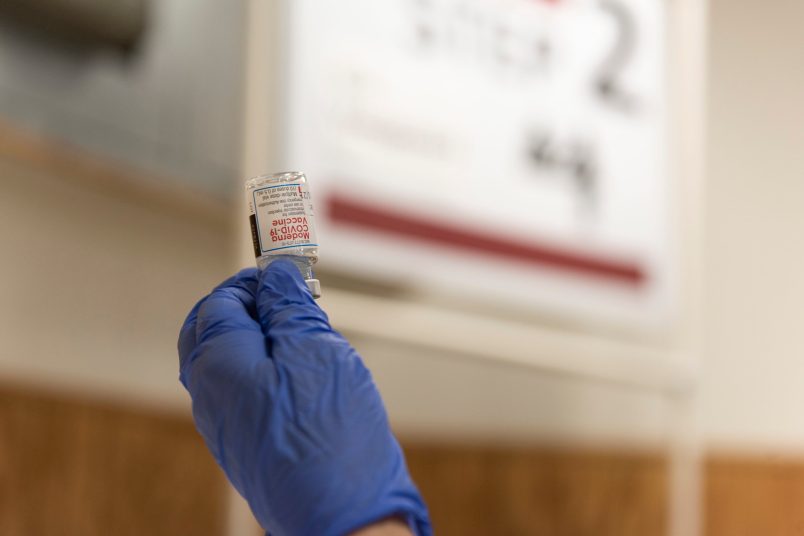




First!
This is my late, great beastie boy. RIP, Feather.
Republicans not only are willing to let people die to maintain their political power; they are also willing to destroy the institutions that support a decent life. Facilities such as hospitals and schools are simply empty buildings if you destroy the professions that make those facilities worthwhile. I can’t imagine anyone wanting to practice medicine under those circumstances.
I have often thought that a good analogy for business was the goose that laid the golden egg. If you prioritize profits over workers, eventually the workers will be unable to purchase the goods they produce. Republicans pursuit of power over everything else will eventually result in the destruction of the support systems that made the power exist. They must think that they will still be able to access the health care and education that they need, but I don’t think those things will be available, even for the elites.Skilled providers of essential services are the goose. Republicans kill it at their peril.
Excellent article!
Interesting cognitive dissonance (emphasis mine)
“Montana is a very good example of a state that has seen consistent undervaccination, and as a result every third life could have been saved,” said the study’s co-author Stefanie Friedhoff, associate professor of health services, policy and practice at the Brown University School of Public Health.
Harkins, the St. Peter’s chief medical officer, is a lifelong Republican. She calls herself “MAGAfan” on Instagram. But she has seen divisions in her own family over the need for vaccines. It’s exhausting and heartbreaking. “It didn’t have to be like this,” she said. “Conservatives are on the wrong side of this.”
What happened in Montana is what happens when right wing media and politicians drive the story. Media hacks should know better than move actively to the side of misinformation and ignorance. Right wing politicians should be driven by a concern for their constituents and not what an uninformed media President says. The right wing media and right wing politicians turned Covid political and thousands upon thousands died. That is America’s eternal shame.
Don’t kid yourself the right wing politicians would have never had the impact they had if the media hadn’t encouraged them.
The GOP is toxic to Earth and everything that lives on it.