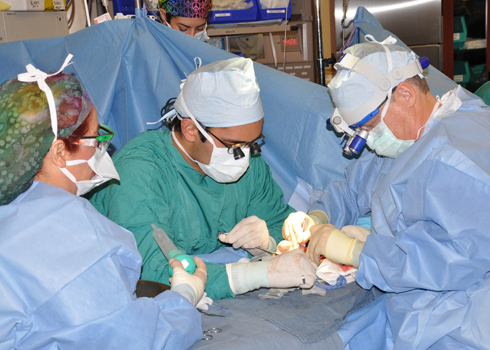
If the health care reform law were to disappear tomorrow, Dallas Wiens would be in trouble.
Earlier this week, in a 15-hour procedure, Boston surgeons grafted a donor’s face onto Wiens’ skull. Weins is a 25-year-old boom lift operator from Texas who came into contact with a live electrical wire, costing him his lips, nose, and eyes and leaving him severely disfigured.
The Department of Defense covered the cost of the surgery through a grant to Brigham and Women’s Hospital, where the surgery was performed — an investment the military hopes will pay off in new surgical techniques that will benefit wounded soldiers. But all the Pentagon’s largesse would have been for naught without the new health care law.
At 25, Wiens was too old to be a beneficiary on his parent’s health insurance policy, until the health care reform law raised the maximum age to 26. Without that coverage, Weins wouldn’t have been able to afford the expensive immunosuppressant drugs that he must take for the rest of his life to prevent his body from rejecting his new face. Patients have to demonstrate that they will be able to afford the anti-rejection drugs to qualify for a transplant.
If the health care reform law were to be wiped off the books before Wiens turns 26, he’d have to figure out, quickly, how to get those drugs by other means. Wiens almost certainly won’t run into trouble. According to the Associated Press he’ll turn 26 in a few weeks, and transfer off his father’s insurance on to Medicare, which covers seniors 65 and older, people with disabilities, and those suffering from a handful of specific life-threatening illnesses.
 But if the Republican Party’s crusade against the health care reform law is successful — if they somehow manage to repeal it, or if the Supreme Court voids it entirely — other transplant patients will find themselves in a similarly perilous situation: with a new organ but unable to afford the critical life-saving drugs that make transplants viable.
But if the Republican Party’s crusade against the health care reform law is successful — if they somehow manage to repeal it, or if the Supreme Court voids it entirely — other transplant patients will find themselves in a similarly perilous situation: with a new organ but unable to afford the critical life-saving drugs that make transplants viable.
In the year since the law passed, patients and their doctors have been making treatment decisions based on current benefits, according to health care experts and providers interviewed by TPM, including the prohibition on discrimination against children with pre-existing health conditions, a “Pre-Existing Condition Insurance Plan” for adults, and the “Young Invincibles” provision that allowed Wiens to get his transplant.
Like Wiens, other patients will get transplants and life-saving treatments, thanks to these new benefits. But, also like Wiens, these same patients will require lifetimes of expensive care and medication, without which they’ll reject their new organs and die, according to the experts and providers we talked to. The consequences of the care they received thanks to the health care reform law, will leave them holding the bag, if Congress or the Court abolishes it. That means bankrupting out of pocket costs, a scramble for care and medication, and possibly death.
Interviews with doctors, patients, and advocates, suggest this is a very real potential consequence of an abrupt, and complete, repeal or voiding of the law.
“Then you’ve got a life and death issue because without those drugs, your organ will be rejected, and when that organ is rejected, unfortunately you will die,” said LaVarne Burton, president of the American Kidney Fund.
Patients with these sorts of life-threatening health conditions wouldn’t necessarily face automatic death sentences if they become ensnared in the politics of health care reform. But their options would be meager, and when they proved inadequate, or didn’t materialize, it could cost them their lives.
“We don’t know how many people will be in that particular situation, and that will depend partially on when patients start getting transplanted under the health care reform regulations, and if it does get repealed, will it happen in one or two years, and how big will the pool of patients be in that time frame,” said Dr. Javed Butler, an Emory University cardiologist, health policy expert, and spokesman for the American Heart Association. “The size of the pool of such individuals will surely grow over time.”
The percentage of all transplant patients who fall into this hole would be small. But, Butler noted, the problem would extend far beyond transplant patients to patients requiring other forms of advanced care. “The numbers will not be minor or minuscule,” he said.
 Butler points to the plight of people with end-stage heart failure. In the past, and in the absence of a donor organ, that diagnosis would have been fatal. Today, doctors can implant what’s known as a Left Ventricular Assist Device into the chest cavity, to mechanically pump blood and ease the strain on the sick heart. (This is the device that former Vice President Dick Cheney, who suffers from congestive heart failure, received last year.) Patients can now survive long term with those devices but require specialized ongoing long-term care.
Butler points to the plight of people with end-stage heart failure. In the past, and in the absence of a donor organ, that diagnosis would have been fatal. Today, doctors can implant what’s known as a Left Ventricular Assist Device into the chest cavity, to mechanically pump blood and ease the strain on the sick heart. (This is the device that former Vice President Dick Cheney, who suffers from congestive heart failure, received last year.) Patients can now survive long term with those devices but require specialized ongoing long-term care.
This is much different than being an organ recipient, Butler said, and “[because] there is no particular limitation in terms of availability, the pool of such individuals could be potentially large.”
The consequences of a change in benefits would exceed the obvious human toll, and include the waste of economic resources, and, in the case of transplant patients, the loss of a viable organ.
Once the benefits were rescinded, patients would have unenviable choices. A transplant patient could apply for Medicaid in his or her state. Some of those between the ages of 18 and 26 could apply for temporary and expensive COBRA benefits. If those options were exhausted, he or she could beg pharmaceutical companies to provide free medication as part of their patient assistance programs. But that’s about it, advocates, experts, and providers say.
To be clear, the phenomenon of people in need of chronic care suddenly finding themselves hobbled and without adequate insurance coverage isn’t new. But it’s typically the result of an unforeseen change in individual circumstances — a layoff, say, or an insurance company rescission — not a wholesale change in the law.
Phil Green is 58 years old, and used to run projects for a private contractor called Continental RPV (Remotely Piloted Vehicles). He would manage and build aerial targets for the military and other countries — target drones used for training gunners.
“I had a real good career and everything else, and one thing led to another where I couldn’t do the job anymore, I lost my insurance, they took me off the transplant list — was on it since 2002,” he told me this week, just after undergoing dialysis.
 Green survives on Medicare, which has a special carveout for people under 65 with end-stage renal disease. Medicare covers his dialysis, but if he gets a kidney transplant, Medicare will only cover his anti-rejection drugs for 36 months, after which he’s on his own. Because Green would be unable to afford those drugs, and Medicare only covers some of the transplant costs, he got booted from the transplant list.
Green survives on Medicare, which has a special carveout for people under 65 with end-stage renal disease. Medicare covers his dialysis, but if he gets a kidney transplant, Medicare will only cover his anti-rejection drugs for 36 months, after which he’s on his own. Because Green would be unable to afford those drugs, and Medicare only covers some of the transplant costs, he got booted from the transplant list.
“They took me off because I’m not financially able to afford the transplant, and the followup medications,” he said. “I’ve kind of given up — I always thought once I get a transplant I can go back to work, doing what I was doing before, everyone in the industry knew me. I’ll go as long as the dialysis works, and then I don’t know because each year gets worse and worse. I always had really good energy … but now I can see that things are going down, down, down.”
When the wars in Iraq and Afghanistan became ground based, Green’s industry contracted. So his employment options are limited. “How do you even begin to look for work in this kind of economy in my condition?” Green wonders aloud.
There are no shortage of stories like Green’s. But they’re caused by fundamental failures of the health care system that the aims to fix. If the law were to disappear in one fell swoop, it would sweep a whole new category of patients into this circumstance, not because of a market failure, but because of politics.
This worst-case scenario would happen only if the law were repealed or thrown out in its entirety by the Supreme Court. Wholesale repeal is unlikely to make it through the Democratic-controlled Senate and would be vetoed by President Obama. The Supreme Court could uphold the law, or strike the insurance mandate provision alone, leaving intact the benefits critical to transplant patients. But according to experts, this is a very real scenario if Republican lawmakers who support immediate repeal of the law were to prevail.
The political and medical fallout, if they got their way, would resemble the unfolding chaos in Arizona, where Republican Gov. Jan Brewer’s Medicaid cuts are leaving patients who’d come to rely on its bare-bones insurance on their death beds — or sticking hospitals, and therefore taxpayers, with the bill.
“That’s a horrible situation and I can’t imagine a single medical center that would let that patient go,” Butler said. “You can’t transplant a patient and let them be without medication.”